
IV Administration Sets and Pumps: A Clinician’s Guide
How to Choose the Right IV Administration Set for Your Facility
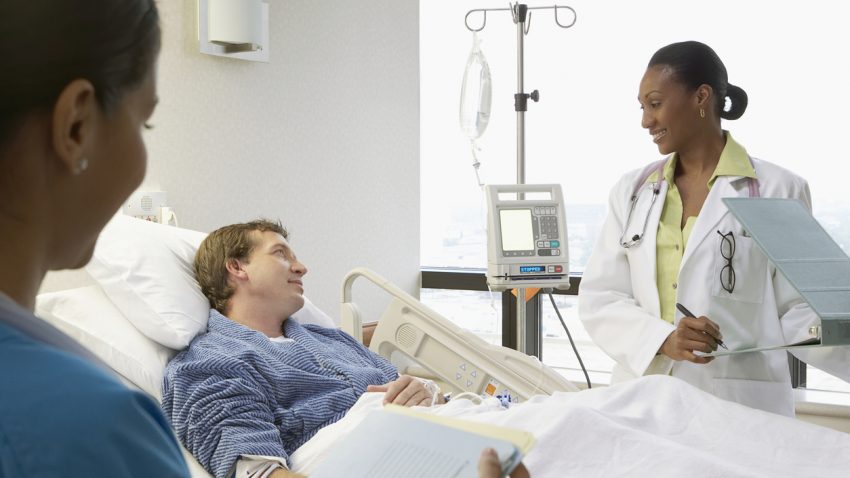
An intravenous (IV) administration set is a medical device used to easily deliver nutrients and medications in a fluid form directly into a patient’s bloodstream for fast results. These commonly used devices are used across a wide range of clinical settings, including hospitals, nursing homes and private domiciles, to deliver a required nutrient and/or medication, such as insulin, hormones, antibiotics, chemotherapy drugs, and pain relievers. IV administration sets allow the user to control the rate, duration and quantity of fluid, minimizing the risk of mistakes and helping make patients feel secure in the knowledge that they are receiving good care.
As a general rule, an IV set includes:
- A sterile container (either a glass / plastic bottle or plastic bag) filled with the required fluid
- An attachment enabling the fluid to leave the container in single drops so that the flow rate can be observed and air bubbles kept to a minimum
- Long, sterile tubing and clamp to allow the control of the flow
- A connector to attach the set to an access device, and
- Y-sets for when a second infusion set needs to be added to the same line.
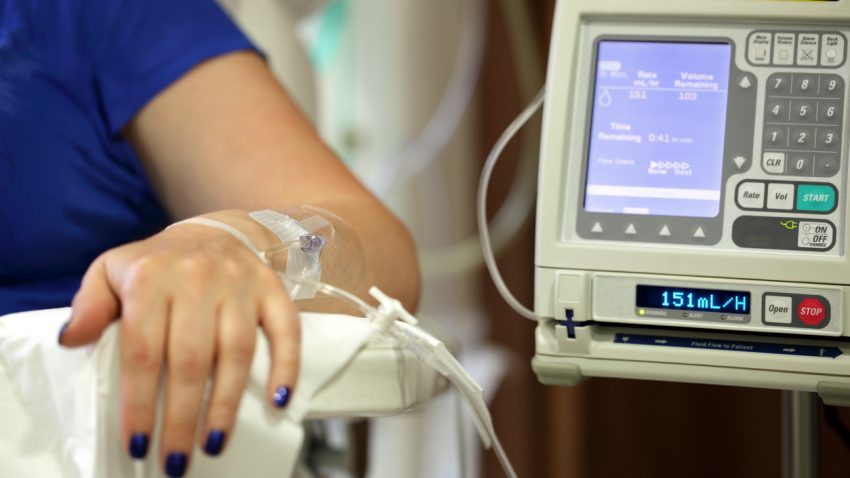
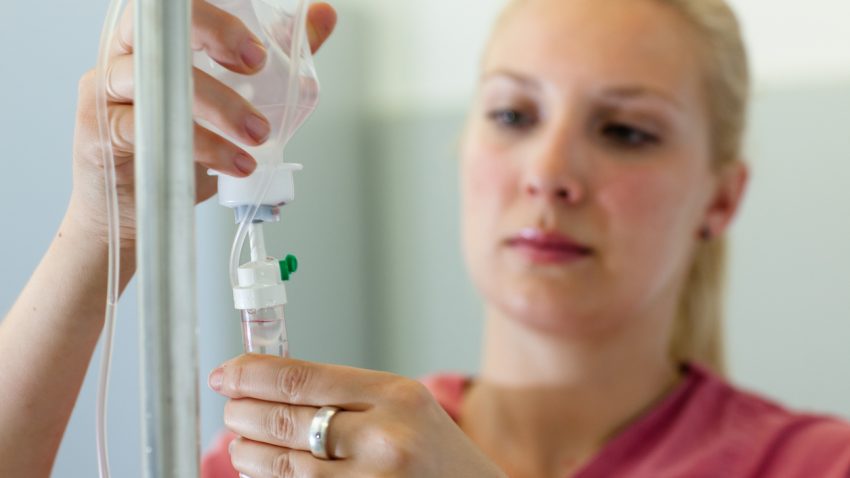
An infusion pump is used to control the exact rate of flow and amount of fluid administered. If a pump is not used, the fluid container is placed above the patient and the clamp used to control the rate of flow, a system known as a ‘gravity drip.’
In this article, we give you a brief history of IV treatments, detailing the development of IV equipment, and cover some of the most frequently asked questions, such as:
- What does IV treatment entail?
- Where it can IV therapy be carried out?
- What are the different types of IV therapy?
- What are the different types of IV pumps?
- And, of course, how you can choose the right IV equipment for your facility.
A Brief History of IV Treatments and Infusions
Intravenous medicine has been around for centuries, with the first recorded use of intravenous delivery dating back as far as 1492. However, it wasn’t until the 17th century that the first working IV infusion prototype was developed in 1658 by English architect, Christopher Wren.[1]
Building upon Wren’s invention, medical scientists experimented further with the intravenous administration of drugs and fluids, developing better needles that enabled the first blood transfusion in 1665. However, some patients lost their lives during these experiments, leading to authorities in the UK, France and the Vatican banning blood transfusions. These bans remained in place for a century, meaning that research into intravenous medicine was impossible during that period.
Once the bans were lifted, research resumed and progress was fast. It was quickly identified that the main issues that surrounded intravenous transfusion were the requirement for a slow and steady delivery, the need to reduce the risk of air embolism, and the aim of preventing volume overload.
The first prototypes of infusion pumps were developed in 19th century, which was a major step towards controlling the rate of flow of intravenous fluids. It was the 20th century that really saw major advances in developing and improving technology, including IV pumps. The need for quality medical care under pressure during the two World Wars provided the impetus for further refinements, including better needles, plastic tubing replacing rubber tubing, and vacuum bottles to reduce the chance of an air embolism. Then in the 1950s, plastic bags began to be used instead of vacuum bottles, further improving the safety and hygiene of the devices.
The late 1950s also saw the introduction of the first ambulatory infusion pump. This was called the Watkins Chrono-Fusor and its main use was in the delivery of Fluorouracil, a chemotherapeutic drug that is still used today in the treatment of cancer. The Chrono-Fusor shared many of the features of modern, programmable devices, including a rotary peristaltic mechanism, and was needed to be wound up with a key, similar to the way that grandfather clocks are powered.
IV Infusions in the 1970s
There was little major change in IV pumps until the 1970s, when a growth in the home infusion market drove a move towards smaller, more affordable devices. This resulted in Deltec Systems (now Smiths Medical MD) releasing the CADD (Computerized Ambulatory Drug Delivery System) pump in the early 1980s. These devices became particularly popular for use in laboratory research involving animals, since they offered a practical solution to the need to deliver drugs in ambulatory animals. Previously, ambulatory IV pumps could only supply a single therapy, meaning that multiple pumps were required for different drugs and rates of pumping.[2]
The early 1990s saw the advent of multiple therapy pumps that were capable of different programming for differing infusions. However, while this was a major advance, it came at a price, since increasing the size and weight of the pumps meant they were less useful when working with animals. As the ‘90s wore on, smaller, lighter IV pumps were developed to combat this problem, such as the CADD Legacy and CADD MICRO. In the mid ‘90s, German inventors released the Pegasus, which was the smallest pump available at the time and was the first to feature computer communications.
Because ambulatory IV pumps were available with PC communication functionality, researchers could track pump data more accurately, as well as examine a pump’s past performance to determine the issues surrounding difficult infusions. The new possibilities opened up by this technology inspired a move towards wireless communication with pumps.
Early wireless devices relied on infrared data transmissions and proprietary RF signals, making them difficult to work with. Modifications to the working environment were required to minimize interference with the transmissions and the pumps were not practical for most scenarios.
As general wireless technology improved, the early 21st century saw the introduction of so-called ‘smart’ pumps. Inspired by the need to minimize the risks to patient safety, these pumps came with the ability to store dosing guidelines within the pump’s memory, meaning that clinicians would receive a warning in the event of potentially unsafe drug deliveries. Smart technology also enabled IV pumps to provide pump history downloads, as well as the ability to be programmed remotely and associated with a specific patient to further reduce the chance of error. Rather than relying on infrared transmissions, these modern devices utilize one of a number of options, including Wi-Fi, Bluetooth, ZIGBEE and Ethernet. Given that most – if not all – healthcare facilities come with the necessary infrastructure to support Wi-Fi, it is unsurprising that Wi-Fi based pumps are proving highly popular, especially since they are easy to access on the wireless LAN, allow the remote downloading of data and can also be set up to issue alerts via email or text.
IV pumps have come a long way over the centuries, transforming IV therapy from a radical experiment to a commonplace treatment used in a wide range of situations, from emergency, life-saving situations through to preventative care. IV therapy is highly versatile and has transformed what were once risky procedures to straightforward routine. This innovation is largely down to the improvements in IV pump technology.
What Is IV Treatment and What Is It Used For?
IV stands for ‘intravenous’ and IV treatment involves delivering required liquids directly into a vein. IV infusions are sometimes called ‘drips’ and are the quickest means to get fluids and drugs into a patient. These can include fluids to counteract dehydration or electrolyte issues, as well as blood transfusions and medications.
There are two different types of IV treatment: infusion and transfusion. Infusion is the term used when an outside substance is introduced to the bloodstream, e.g. medication, while transfusion is when the same type of substance but from an outside source is introduced, e.g. blood or plasma transfusion.[3]
There are a number of reasons why someone might need IV treatment. Sometimes, when someone is suffering from a complex disease, they cannot eat and taking oral medication becomes impossible. Another reason is that some medications are inappropriate for oral administration because the acidic digestive system will break them down before they can be absorbed by the body to treat the disease. In acute care situations, treatment needs to be immediate, and IV delivery is much faster than oral medications. In addition, if a patient is unconscious, IV therapy means that they can still be treated.
Originally, IV treatment was carried out solely in hospitals, but as the range of IV pumps expanded to include ambulatory pumps and lightweight pumps, IV therapy can also be given in outpatient infusion therapy centers or even in the home under the supervision of specialized nurses.
The list of conditions that may see IV therapy utilized is long and includes:
- Cancer and the associated pain
- Gastrointestinal tract diseases
- Dehydration due to nausea, vomiting and/or diarrhea
- Chrohn’s disease
- Multiple sclerosis
- Certain types of arthritis
- Congestive heart failure
- Certain types of immune deficiency disorders
- Some congenital conditions
- Childbirth, e.g. epidural.
When Can IV Therapy Be Carried Out In the Home?
A need to minimize healthcare costs combined with improvements in technology led to the possibility of receiving IV therapy outside of a hospital environment. Individuals who face long-term therapy will also face expensive inpatient care as well as difficulty in enjoying a normal lifestyle and going back to work.
It has long been recognized that psychological well being plays an enormous role in a patient’s prognosis. Most patients prefer to stay at home where possible and this is a major factor in the development of home IV therapy, which provides a highly cost-effective alternative to hospital treatment.
Before home IV therapy can proceed, both the patient and their home are thoroughly assessed to determine whether the patient is a good candidate for home treatment. The therapy is then overseen by a qualified physician, who will issue a prescription order for an infusion therapy provider to fill out. Such home infusion therapy pharmacies are state-licensed and have received specific training in the provision of IV home therapies. They must also meet a number of regulatory requirements as laid out by state pharmacy boards and appropriate accreditation standards. In addition to supplying IV medications, they may also supplies related therapies and services, such as enteral nutrition therapy, inhalation therapy, and care management. Some home infusion therapy pharmacies are independent, while others are affiliated with selected healthcare providers, such as hospitals, home nursing agencies, and other pharmacies.
What Other Alternatives Are Available for IV Therapy Outside a Hospital Setting?
In addition to home treatment, patients may be able to visit an ambulatory infusion center for their IV treatment. A number of home infusion therapy providers also offer an AIS (Ambulatory Infusion Suite of the home infusion therapy provider), where clinical care in accordance with a doctor’s orders can be carried out by RNs and registered pharmacists that have specialized skills in the administration of IV treatment. This offers a very cost-effective alternative to hospital treatment and provides another alternative to patients who are appropriate candidates for this approach.
An AIS is one of three different types of ambulatory infusion centers, the others being physician-based infusion clinics and hospital-based infusion clinics.
What are the different types of IV?
IVs are categorized by the type of vein being used. The IV tube is called a catheter and may be inserted into a number of locations across the body according to need.
Peripheral IVs are the most commonly used IV therapy and, as the name would suggest, are used with peripheral veins, i.e. the veins found in the arms, hands, legs and feet.
Central IV lines involve the catheter being inserted through a vein and then empties into a large vein within the torso, such as the superior vena cava, or the inferior vena cava. Since these veins are larger than peripheral veins and subsequently have a faster blood flow, central IVs are preferred for fluids that may irritate the lining of the blood vessels, such as chemotherapy medication. In addition, central IVs offer a fast distribution throughout the body, due to the delivery of medication close to the heart, and they allow for the delivery of multiple medications, since the catheter is large enough to accommodate multiple parallel compartments known as lumen. Another advantage is that central IVs enable the measurement of central venous pressure and other variables.
However, central IVs also have a number of associated risks, including bleeding, infection, gas embolism, and thromboembolism. A skilled clinician needs to insert them, since the required veins can be difficult to find, and there is the possibility of damage to parts of the body, such as the carotid artery or pleura if the IV is not appropriately sited.
There are a number of different types of central IVs according to where the catheter is placed. For example, PICC lines are placed through a sheath into a peripheral vein before being guided upwards to the superior vena cava or right atrium. Once in situ, they are normally used when long term therapy is required, e.g. chemotherapy, antibiotic therapy or total parenteral nutrition. Once in place, a PICC line can be left for months or even years without needing to be replaced. While a PICC line carries with it an increased risk of infection if bacteria enter the body through the catheter, it is less risky than other types of central IVs, since the insertion site is generally cooler and dryer, which means that the rate of bacterial growth is lower than with other central IVs.
Another type of central line is a tunneled catheter, which is when the catheter is inserted through the skin and are then ‘tunneled’ a distance before reaching the vein. This method of IV therapy minimizes the risk of infection since there is no chance of bacteria on the skin entering the vein.
A ‘port’ is a central venous line with a small, silicone covered reservoir attached instead of an external connector. Frequently called by a brand name, e.g. MediPort or Port-a-Cath, ports are implanted beneath the skin, where it can be left for a long period of time, years even. The reservoir is filled with medication on a regular basis by injecting drugs through the silicone, which is self-sealing. This silicone cover is capable of undergoing hundreds of piercings while maintaining its integrity. If a port will be left in a patient for the long term, it will need to be flushed with an anti-coagulant on a monthly basis to avoid it getting plugged up, which carries with it a potential risk of embolization.
Installing a port is a complex process that requires a skilled clinician, although once in place, they are usually easily removed as an outpatient procedure. Given how convenient it is for the patient to have a port in place and the fact that they have a lower risk of infection that PICCs, they are generally the IV therapy of choice for patients requiring long term intermittent treatment.
Finally, another type of IV therapy is a midline catheter. Like a peripheral IV, a midline catheter is inserted into a peripheral vein, but they advance further through the vein than a peripheral IV, although a midline catheter does not go as far as a central vein.
What are the types of IV transfusion?
There are three main types of IV transfusion.
- Continuous or intermittent infusion. This is mainly used with patients suffering from fluid and/or electrolyte imbalances. This is in contrast to those situations when medication is only needed intermittently, which would require secondary IV or IV push.
- Secondary IV. The tubing that connects the bag of fluid to the patient is known as the primary tubing. When an additional IV is attached to this tubing, this is a secondary IV. (Sometimes called IV piggyback.) This is a preferred option to placing multiple catheters. When a secondary IV medication is given, the primary bag is stored lower than the secondary bag so that medication from the secondary bag can flow directly into the primary tubing without the secondary tubing being contaminated with fluid from the primary bag. The fluid from the primary bag is then used to flush through any residue from the secondary IV.
- IV push. This is when a syringe containing medication is connected to an access port sited in the primary tubing so that the medication can be delivered through the port. The syringe plunger must be pushed in slowly to avoid irritating the vein or administering the medication too quickly. Once the medication is in the fluid stream of the IV tubing, it is frequently followed with a second fluid injection, known as a ‘flush’, to ensure that the medicine reaches the bloodstream as expected. An IV push is not suitable for all medications, e.g. potassium should never be given via IV push since the resulting spike in medication levels could prove fatal to the patient.
What Are The Different Types of IV Pumps?
As outlined in the history of IV pumps, this technology was developed to enable the administration of fluids that would be difficult and/or expensive to deliver manually by medical professionals. IV pumps are sensitive enough to be able to deliver amounts as small as 0.1 mL of fluid per hour, which is too small to be given via a drip. They can be programmed to deliver medication every minute, or to deliver different volumes of fluid at different times, all of which is much more cost effective when controlled by an IV pump as opposed to paying for staff members to administer.
What Types of Infusion Can IV Pumps Control?
IV pumps can be programmed by an appropriate medical professional to deliver a wide range of infusion types. These include:
- Continuous infusion, consisting of regular pulses of infusion, generally between 500 nanoliters and 10 milliliters. The pulse rate can be programmed to a specific speed.
- Intermittent infusion, consisting of periods of high infusion rates alternated with low rates so that the cannula remains open. The length of these periods is preprogrammed.
- Patient controlled infusion, which allows patients to choose the rate of medication delivery. This type of confusion usually has a predetermined maximum delivery rate to avoid the possibility of an overdose and the patient simply has to press a pad or button when they feel the need. This is a very common infusion type for patient-controlled analgesia (PCA) which offers patients the ability to be in control of their pain management.
- Total parenteral nutrition, which is a long term infusion treatment that necessitates a schedule approximating normal mealtimes.
- Pumps that allow for a variation in delivery according to the time of day, which takes into consideration the circadian cycles required with certain categories of medication.
What Types of IV Pumps Are Available?
There are two main classes of pump: large-volume; and small-volume. Large-volume pumps are designed to deliver large nutrient solutions while small-volume pumps are used for hormones, e.g. insulin, and medications, e.g. analgesia. However, there is a lot of deviation within these two classes. Some pumps are small enough to be portable, while others are larger and for use in a hospital environment. There are also specialized IV pumps for charity and battlefield use.
Large-volume pumps usually use a variation of a peristaltic pump, with computer-controlled rollers squeezing the tubing to push through the fluids. Alternatively, some types utilize a series of fingers, pressing on the tube in order to keep the fluids moving.
Small-volume pumps, on the other hand, frequently have a computer-controlled motor that turns a screw which then pushes down the plunger on a syringe. Some of the smallest devices work on the basis of osmosis. They utilize a bag of salt solution, which absorbs water across a membrane, forcing out the medicine. The rate of deliver is carefully controlled through alterations in the salt concentrations and pump volume. These types of pumps are generally recharged with a syringe.
Although modern innovations are constantly incorporated in new IV pump technology, some devices rely on older techniques. Clockwork pumps are still used when working with animals and for portable small-volume pumps. These IV pumps usually contain one spring to control the infusion and another to trigger an alarm when the infusion is finished.
What Are the Side Effects of IV Therapy?
Although IV therapy is safe for most people, like any type of medication, there is a risk of side effects that range from mild to life threatening. This is why it is advised that anyone who is facing IV treatment should discuss this option thoroughly with their clinician so that they are fully aware of how long their IV treatment is likely to last and what their risk is of any particular side effect.
One of the advantages of IV therapy is that it allows medication to take effect very swiftly. However, this also means that any negative side effects or allergic reactions can also occur quickly. Given this fact, patients are usually observed for the duration of their infusion and may also be for a while after the infusion is finished.
The most common side effects from IV therapy include:
- Infection: The injection site may become infected. To minimize this happening, the IV therapy must be administered carefully with completely sterile equipment. Many systems come with disposable components to support this practice. If the injection site becomes infected, this can also cross into the bloodstream, leading to a serious infection. Symptoms of an infection may include raised temperature, chills, redness, soreness, and inflammation at the injection site. If a patient suffers from any of these symptoms they are advised to contact their physician immediately.
- Damage to blood vessels: If an IV catheter is poorly inserted, this can damage veins causing infiltration. If a vein is damaged, this may result in medication leaking into the surrounding tissue instead of entering the bloodstream as intended. Infiltration may also result in tissue damage. Other possible side effects are phlebitis (inflammation of the veins). If a patient is suffering from infiltration and/or phlebitis, they may experience warmth, pain and inflammation at the injection site. If this is the case, they should contact their doctor immediately.
- Air embolism: Although a small amount of air will not cause any concerns, if an air bubble gets into the syringe or medication bag or the line is allowed to run dry, air bubbles can go into the patient’s vein, before traveling to the heart or lungs, blocking blood flow. In the worst case scenario, this can cause major problems, including heart attack or stroke.
- Blood clots: IV therapy may result in the formation of blood clots, which can then block major blood vessels, giving rise to tissue damage or even death. Deep vein thrombosis (DVT) is an example of the type of serious blood clot that may be caused by IV treatment.
What Are the Safety Issues Surrounding IV Pumps?
Over the period 2005-9 there were over 56,000 adverse event reports arising from the use of IV pumps. This figure includes at least 500 deaths. This lead to the U.S. Food and Drug Administration (FDA) to put into place the Infusion Pump Improvement Initiative to improve IV pump safety.[4] The initiative identified the main causes of adverse events to be software issues, user interface problems and device failure.
There are a range of safety features that have been developed for IV pumps that attempt to address potential problems to minimize their risk. Different pumps contain different features depending on the age and make of the IV pump. These include:
- No single point of failure. This is a legal requirement for all human-rated IV pumps regardless of age, although veterinary infusion pumps are exempt from this requirement. This means that there should be no single cause of failure that would make the pump silently fail to operate.
- A battery backup to maintain the rate of transfusion in the event of a power failure or the device is accidentally unplugged.
- Anti-free-flow mechanisms to avoid blood drainage from the patient and prevent infusate entering the patient unregulated while the IV pump is being sited.
- A down pressure sensor to alert staff if a patient’s vein or the line is blocked and an up pressure sensor for when the bag or syringe is empty or is being squeezed.
- An air-in-line detector. Some pumps have the capability of measuring the volume of air in the line from 0.1 to 2 ml of air. Although amounts this small will not harm the patient, they can interfere with the effective transmission of low-dose medicines.
- A built-in drug library with customizable programming to allow the device to be tailored for specific drugs to avoid medication errors.
- The ability to keep a log of time stamped therapy events for data analysis. Most IV pump logs require a security code to be inputted before a log can be deleted to protect abuse of a patient or the device.
- The ability to configure the display so that only certain features are displayed during operation so that patients, untrained staff, or visitors do not accidentally interfere with the workings of the device.
How to Choose the Right IV Administration Equipment For Your Facility
Advances in IV administration technology means that there is an overwhelming array of choice when it comes to IV pumps. It can be difficult to choose the right equipment for your facility, even allowing for purchasing multiple different devices.
When deciding upon which IV administration equipment to purchase, a number of factors should be considered. These include the types of fluids that need to be administered – if you need to deliver nutrients, then you need to consider large-volume pumps. If you have a need to administer hormones or medication, you will need small-volume pumps. Given the potential safety issues associated with IV pumps and the responsibility of healthcare facilities to prioritize patient safety, pay careful attention to the safety features with any given device to determine if they offer the support you need.

Infusion pumps, left to right: Baxter FloGard 6201, Braun Vista® basic Large Volume Infusion Pump, Baxter Sigma Spectrum Infusion Pump
Some of the most popular pumps from leading suppliers include:
- The Baxter Flogard, which is a volumetric infusion pump capable of handling a variety of fluid types at various infusion rates. It comes with a range of functions for ease of use, designed with safety in mind. For example, the side clamp option protects against the possibility of unwanted gravity free flow, while the front panel is lockable to prevent tampering. It allows for the piggybacking of additional medications and the programmable delivery profile can handle up to ten steps, giving full control of infusion ramping and tapering.
- The Braun Vista® basic is an IV pump has sold over 100,000 units across the world, a testament to its simplicity of use combined with reliable results. It comes with all the features required for mosts situations, including continuous, piggyback and program mode, and is designed to provide consistent performance for many years, with the battery lasting for 3 years before requiring replacement. Available with both DEHP-free sets and needle-free sets for patient and clinician protection, it is suitable for use in a range of settings, including the home, due to how easy it is for users to program and use.
- The Baxter Sigma Spectrum Infusion System allows for auto-documentation, freeing up nursing staff time. A patient using a Sigma Spectrum Infusion System will have their infusion data automatically added to their electronic medical record, ensuring accurate information at all times. The system also provides automatic wireless drug library updates without the need for staff input so that the drug library is always relevant and effective. A small, lightweight pump, it is easy to carry around and its large font and user-friendly on-screen help make it simple to program necessary infusions.
The Baxter Flogard and Sigma Spectrum and Braun Vista are all pole mounted pumps.
If you require an ambulatory pumps, some of the leading options are:
- The CADD-Legacy® PLUS pump from Smiths Medical. With its easily understood display screen, this reliable pump comes with the facility to download relevant event history to a PC either directly or remotely via a modem. It has a number of safety features, including occulsion sensors for both upstream and downstream low so that there is an immediate alert in the event of a problem with fluid delivery, as well as an air-in-line detector to warn of any air in the tubing. It can be programmed with an infusion rate of up to 125 mL/hr at a volume of up to 1,000 mL, so it can accommodate a wide range of therapies and has an internal clock so that dosing remains on schedule.
- The Smiths Medical Cadd Prizm Deltec. This ambulatory infusion pump is designed for single therapy use and comes with an integral data port to enable the device to interface with a printer or modem or connect to a remote dose cord. The pump can be programmed remotely via a modem. The Model 6101 version has an occlusion detector that can sense both upstream and downstream blockages and offers customizable programming features, as well as an alert to warn when the pump is due for maintenance.
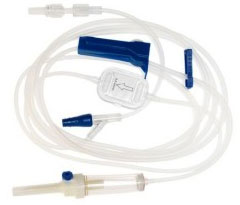 Baxter, Braun and Smiths Medical all recommend that their brand-name tubing is used with their pumps, although there is compatible tubing available at a discounted price from trusted brands such as TrueCare Biomedix, HLIC and Acta Medical.
Baxter, Braun and Smiths Medical all recommend that their brand-name tubing is used with their pumps, although there is compatible tubing available at a discounted price from trusted brands such as TrueCare Biomedix, HLIC and Acta Medical.
These are just a few examples of the pumps that are available to healthcare facilities. If you have difficulty determining which IV system to use, make a list of the features you require and prioritize them in order of importance, making sure to determine your ‘must-haves’. Cross reference this against your available budget to help narrow down your choices.
The Future of IV Pumps
The technology surrounding IV pumps continues to improve and we have yet to see what else these valuable devices have to offer when it comes to best practice healthcare. They continue to perform an important function in the delivery of essential fluids and medications and it is essential that every healthcare facility stay abreast of the latest developments in order to continue to provide the best and safest possible healthcare.
What has been your experience with IV pumps? What are the most important features for you? What would improve their functionality for you? Let us know in the comments.
Sources:
[1] http://www.ivnnz.co.nz/files/file/7748/Intravenous%20Therapy%20%20Then%20and%20Now%20%20July%202013.pdf
[2] https://www.alnmag.com/article/2008/10/infusion-technology-past-present-and-future
[3] https://medicorx.com/infusion-versus-transfusion/
[4] http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/GeneralHospitalDevicesandSupplies/InfusionPumps/ucm205424.htm
https://www.hospira.com/en/products_and_services/iv_emr_integration